In 1957 I moved to The New York Hospital to fill Norton's place when he moved to Florida. The Schepens Retina Associates and the Eye Research Institute acquired a national reputation for excellence in attaching the retina. I went back to Boston periodically in the first years to confer with the expanding retina group, which added Regan and McMeel, and then Freeman, Pruett, Tolentino, Hirose, and Trempe. Dr Devoe, an erudite chairman and cataract surgeon, viewed our drawings to the ora with skepticism. I returned to Bellevue with a binocular indirect scope-it was 1 of 3 in New York-and I taught the residents to use it. To this day, it remains a common addition to most procedures for retinal detachment. It also preserved the barrier concept for any undiscovered breaks in the periphery. Dr Schepens maintained that it served to counter future vitreous traction. Encirclement was no longer needed, but it was so embedded in our technique that it was retained. 4 Eventually, it became apparent that we should buckle the anterior end of the break as well as the posterior end, and for this purpose numerous silicone forms ( Figure 8) were developed to buckle completely breaks of all sizes and shapes. 
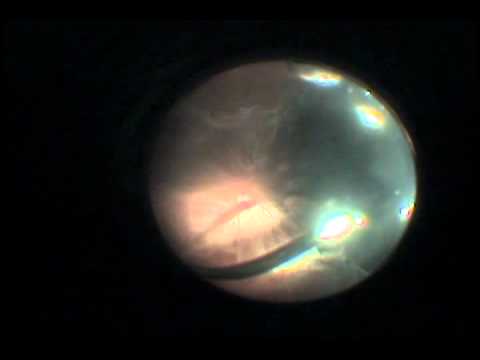
The solution was a 360° buckle the encircling buckle was a pragmatic solution to the anterior leak ( Figure 7). Still, in a number of eyes the anterior leak would circumvent the extent of the buckle ( Figure 6B). To counter this, Dr Schepens extended the buckle to 180° and made several radial lines of coagulation to the ora ( Figure 6A). In the presence of a larger break, however, the anterior end of the break would leak anteriorly and redetach the retina ( Figure 5B). 3 It succeeded in most eyes with small breaks that were supported by the buckle ( Figure 5A). Then he made a lamellar dissection centered on the mark, applied multiple rows of diathermy posterior to the break, and inserted a section of polyethylene tube to create a buckle to augment the diathermy barrier that was intended to prevent a leak from the retinal break detaching the posterior retina ( Figure 4). I can remember standing behind Dr Schepens at the operating table and peering over his shoulder as he localized and marked the posterior edge of a break. The drawings were taken to the operating room and hung adjacent to the table for reference of the meridian and anterior posterior position of the retinal break. Retinal detachment was operated upon under general anesthesia. The scallop at the border indicated that you had seen the ora seratta if a segment was missing, you looked for it at the operating table with more scleral depression. 1, 2 The drawings were in a color code ( Figure 3): red for attached retina and arteries, blue for detached retina and veins, green for opacities in the media, and yellow for exudate. In Boston, when I wasn't working with Dr Cogan in the Howe Laboratory, I would slip downstairs to the retinal clinic to watch Drs Schepens, Okamura, and Brockhurst, using indirect ophthalmoscopy through a binocular scope ( Figure 2) that Drs Schepens and Pomerantzev had developed, draw the fundus and retinal detachment to the ora serrata and find the retinal breaks. Twenty-five days in the hospital for a retinal detachment was not uncommon. The routine was prolonged bed rest with binocular occlusion and then the application of perforating diathermy to the posterior edge of the detachment and drainage of subretinal fluid, followed by more binocular occlusion and bed rest. We knew there was supposed to be a retinal break, but as the breaks tended to be in the periphery and we only used direct ophthalmoscopy, we rarely found them. 
At Bellevue it was assigned to a junior resident for repair. Retinal detachment was a neglected disorder at Bellevue Hospital where I trained, as well as elsewhere in the United States. A leading retinal surgeon in New York-there were 2-referred to him as Boston Charlie, a takeoff on Boston Blackie, a fictional gangster in the movies. Charles Schepens' reputation for treating and curing retinal detachments had reached New York, and there was disbelief. Just before I left for Boston, Edward Norton, a friend at the New York Hospital, advised me to look in on Dr Schepens while in Boston. Dr Schepens had emigrated to the United States and to the Howe Laboratory from London 8 years before. I met Charles Schepens ( Figure 1) in 1955 when I was sent to the Howe Laboratory in Boston for a Heed fellowship with David Cogan. I would like to thank The Retinal Research Foundation, The Schepens International Society, and Alice McPherson for establishing this lecture to honor Charles Schepens and for inviting me to be the first lecturer. Shared Decision Making and Communication.Scientific Discovery and the Future of Medicine.Health Care Economics, Insurance, Payment.Clinical Implications of Basic Neuroscience.Challenges in Clinical Electrocardiography.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
